before leaving
This is a very important section of our blog. On this page we will cover important aspects of the journey concerning the mere bureaucracy up to vaccines with lots of useful tips to read carefully before leaving!

Travel documents
Is the passport still valid? Do we need visas or vaccines in the new country I would like to visit? Did I take travel insurance?
Vaccines
Can I leave peacefully? Have I checked for any recommended or even mandatory vaccines?
travel documents

Passaport: must be valid. All the necessary information can be found easily by asking State Police. If you do not have it or have to renew it, generally in two or three weeks you should have your document in order.
Visa. There are specialized offices that deal with giving you all the information and carry out all the necessary procedures. However, you can always call the consulate or embassy concerned and do everything without intermediaries.


Vaccinations. At the Office of Hygiene you can find a department used for international vaccinations; the doctors in charge provide all the necessary information and in a short time they make the appropriate bites.
Money. We always use the credit card (prepaid) and we usually withdraw directly from the various ATMs at the airport. However, it is important to have a few dollars or euros in stock and well hidden (to be used in an emergency).


Medical insurance. Fundamental. By now there are many and all online, so in a few mouse clicks you can buy the one that most closely matches your needs and, consequently, start with a different mental serenity.
Flight ticket. First of all we usually do a quick check on one of the many online price comparators. We look for the best compromise between schedules and stopovers and, when possible, for greater security, we buy directly on the website of the chosen airline avoiding intermediaries.

vaccines
"Before leaving for an international trip (for tourism, work, study, volunteering, etc.) it is necessary to know your own vaccination situation in order to evaluate the need or not to undertake a personal vaccination plan that takes into account not only the state of general health, including the destination, type and duration of the trip.
Remember that some diseases, long eliminated in Italy, are still endemic or epidemic in some countries.
It is always advisable to consult your doctor before leaving.
The existence of particular conditions, including therapeutic regimens or pregnancy, could, in fact, advise against traveling to areas with climatic and environmental situations different from the usual ones, or contraindicating pharmacological or vaccine prophylaxis ".
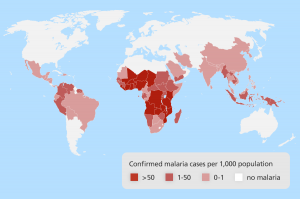
 Malaria
Malaria
Malaria is an infectious disease caused by parasites carried by humans from mosquitoes. It is estimated that this malaria causes 1 million deaths a year, most of them in Sub-Saharan Africa. Pregnant women and children are particularly at risk of serious consequences. The symptoms are fever with chills, sweating, headache, muscle aches, back pain, cough, nausea, vomiting and diarrhea. It is transmitted always and only through contagion of mosquitoes, never due to direct inter-human infection. There are currently no malaria vaccines.
Prevention is possible by taking certain drugs, under the supervision of a doctor, and by adopting certain behaviors such as: the use of mosquito nets, skin and environmental repellents and the use of suitable clothing.
The geographical areas at greatest risk of malaria are most of the African regions, except in altitude; the Amazon basin, in Latin America and some rural parts of South-East Asia.
Prevent insect-borne diseases
Here are the personal prevention measures against insects, formulated by the Ministry of Health:
- avoid if possible to go out between sunset and dawn;
- wear light-colored clothes with long sleeves and long pants;
- avoid the use of perfumes;
- apply insect repellents to exposed skin, repeating the application every 2-3 hours, in case of intense sweating;
- preferably stay in rooms with air conditioning or at least mosquito nets on the windows;
- use mosquito nets over the bed, soaking them with insecticides;
- spray pyrethrum and permethrin-based insecticides in the living room and bedrooms, paying attention to children or indoors.
Prevent foodborne diseases
The World Health Organization suggests the following points:
- choose products that have undergone suitable treatments to ensure their safety (for example pasteurized milk);
- cook the food well and consume it immediately after cooking; otherwise store them immediately in the fridge for a limited time;
- heat any previously cooked food quickly and at high temperature;
- avoid any contact between raw and cooked foods;
- take particular care of hand hygiene;
- thoroughly clean all kitchen surfaces, utensils and containers;
- protect food from insects, rodents and other animals;
- use only drinking water.
As for the vaccinations during the trip planning phase, it is necessary to contact the ASL International Prophylaxis and Vaccination Center in the area of residence: this structure has the task of protecting the health of those about to leave and to give information on how much should be done.
There is a new drug, called Eurartesim della Sigmatau, which serves as a therapy if one realizes that he has contracted malaria while traveling and is given taking 3 pills a day for 3 days in a row. The pack contains 12 pills.
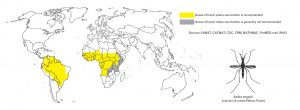
 Yellow fever
Yellow fever
In some countries it is mandatory, in many others it is required only to travelers from infected areas (endemic for yellow fever). The disease is endemic in most African countries and in the northern countries of South America.
It is definitely advisable for travelers to get vaccinated if they go to countries at risk.
In recent years there have been epidemics in Ghana, Nigeria, Senegal, Kenya, Cameroon, Mali, Mauritania, Ivory Coast. Vaccination is 100% effective, while the fatality rate is 60% higher in non-immune subjects.
The vaccination must be made, at least 10 days before departure, in the Centers authorized by the Ministry of Health and notified on the International Vaccination Certificate which must be taken with you during the trip.
Vaccination is not recommended for pregnant women, children under the age of 6 months, immunosuppressed and subjects with a clear allergy to eggs.
 Typhoid fever
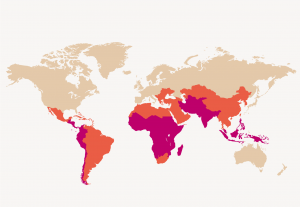
Typhoid fever
All travelers who go to areas where typhoid fever is endemic are at potential risk, although this is generally limited in tourist centers and business centers where housing conditions, sanitary conditions and food hygiene are good . The risk is particularly important in the Indian sub-continent. Even vaccinated people should avoid consuming potentially contaminated food and water.
Vaccine
To travelers who travel to countries where the risk of typhoid fever is high, especially if their stay lasts more than a month or takes place in conditions of mediocre hygiene or those who go to the Indian sub-continent and countries where there may be the possibility of resistance of the micro-organisms to antibiotics, one or the other of the following vaccines will be recommended:
• The Ty21a oral vaccine. This vaccine containing live germs of the attenuated Ty21a mutant strain of Salmonella tiphi presented in liquid form or in gastro-resistant capsules is administered orally in three doses (four in the United States of America) at two-day interval and immunity appears seven days after the last dose. The protection rate is still 67% seven years after the last dose in the inhabitants of endemic areas, but may be lower in travelers.
• Injectable vaccine Vi CPS. The capsular polysaccharide-based vaccine (Vi CPS) containing 25 mg of polysaccharide per dose is administered as a single dose intramuscularly. Immunity appears seven days after the injection. In endemic countries, the protection rate is 72% after one and a half years and 50% after three years.
The two vaccines, safe and effective, have been approved and are currently available. They offer an alternative solution to old whole-germ anti-phaeoidine vaccines that are poorly tolerated. However, their efficacy in children under the age of two is unproven. There is a combined typhoid anti-hepatitis A vaccine.
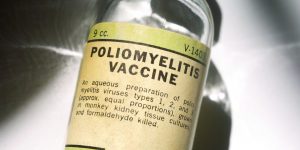 Polio
Polio
The polio vaccine is an inactivated vaccine (obtained with killed viruses) that is administered intramuscularly. It can be given together with other vaccinations.
In children the primary cycle is usually carried out with the so-called hexavalent vaccine (because it contains 6 vaccines: Diphtheria-Tetanus-Pertussis, Polio, Hib and Hepatitis B).
 Diphtheria
Diphtheria
The anti-diphtheria vaccine is made up of diphtheria anatoxin, that is, from the original toxin made harmless by chemical procedures that retain its ability to stimulate the production of protective antibodies. The vaccination calendar, in force since 1999, foresees three doses in the first year of life (at the 3rd, 5th and 12th month), followed by two reminders of 5-6 years, and 11 and 15 years respectively. Further reminders are recommended every ten years.
Diphtheria vaccines are available in pediatric and adult formulations. The pediatric formulation is used for the primary cycle and the calls up to 6 years of age.
The adult formulation has a lower anatoxin content than the pediatric one and is used for booster doses over 6 years and for vaccination of adolescents and adults.
After completing the cycle, the anti-diphtheria vaccination gives almost total protection.
The duration of the protection over time is very long and is further guaranteed by the execution of the calls.
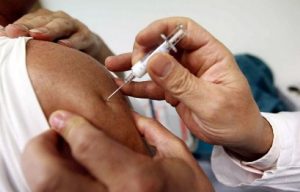 Tetanus
Tetanus
The tetanus vaccine, available in Italy from the early forties, is made up of tetanus anatoxin, that is, from the original toxin made harmless by chemical procedures that retain its ability to stimulate the production of protective antibodies (similarly to what happens with diphtheria anatoxin ).
The tetanus vaccine is usually combined with the diphtheria vaccine, which is shared by the method and timing of administration, and with the acellular pertussis vaccine (DTaP).
For the immunization of newborns, usually today, the hexavalent vaccine is used, which in addition to protecting against tetanus also prevents diphtheria, poliomyelitis, viral hepatitis B, pertussis and invasive HIB infections.
 Rabies
Rabies
The vaccine consists of an inactivated rabbi virus (killed), cultivated on human diploid cells (HDCV) or on adsorbed diploid cells (RVA) or in a chicken embryo (less practiced vaccination) and should be administered subcutaneously deep or intramuscularly.
The pre-exposure vaccination is carried out with the administration of 2 doses of vaccine at a distance of one month from the other; if you want a rapid immunization the vaccination cycle is at times 0, 7, 28 days. In both cases a reminder should be made after a year. Should the risk persist, recalls should be given every 3 years.
Post-exposure prophylaxis is performed possibly within 24 hours in case of suspicious animal bite.
Finally, if you are bitten by a suspect animal and you are vaccinated, it is advisable to take two booster doses in three days to increase the rate of antibody titre increase.
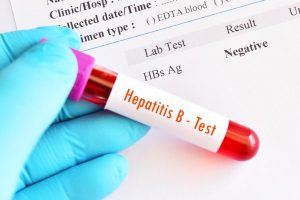 Hepatitis B
Hepatitis B
Vaccination is recommended for all travelers, for long-term residents in highly endemic countries and for tourists who go to highly endemic areas and who intend to live in close contact with the local population or still have sex. The percentage of carriers of the virus is decidedly high (5-20%) in all socio-economic groups in certain geographical areas, such as: Africa, South East Asia, the Middle East (with the exception of Israel), the Pacific islands, the Amazon and certain parts of the Caribbean such as Haiti and the Dominican Republic.
The hepatitis B vaccine is very safe and effective. Optimal protection is already available after the third dose. The vaccination should begin six months before the trip to complete the cycle before departure. The vaccination series must however be started before departure, even if it is not possible to complete it.
 Japanese Encephalitis
Japanese Encephalitis
All travelers who plan to spend at least two weeks in endemic rural areas are candidates for vaccination. Many exposed people must be strongly encouraged to get vaccinated. Currently, three types of Japanese anti-encephalitis vaccine are manufactured and used on a large scale: the inactivated vaccine prepared on mouse brains, the inactivated vaccine prepared in cell culture and the attenuated living vaccine prepared in cell culture. Only the first is widely distributed on the market.
 Cholera
Cholera
No country requires an anti-Chinese vaccination to enter its territory. The two new anti-cholera vaccines (live and killed) administered orally are safe and effective. Approved and distributed on the market in a small number of countries, they are available to travelers who travel to an endemic region where they will be particularly exposed to risk. The vaccine killed confers an important immunity (85-90%) during the six months following the second dose.
The level of protection still reaches 62% at the end of the three years in people over the age of five. The anti-cholera vaccine killed offers, to some extent, a cross-protection against Escherichia coli, that is to say against the traveler's diarrhea. The classic injectable vaccine confers only partial, uncertain and short-term protection and is therefore not recommended.
 Meningitis
Meningitis
Vaccination is highly recommended for all travelers who travel to African countries where the disease is endemic and who live in close contact with the local population. It is a geographical area that extends from Senegal to Ethiopia.
In this area there are often epidemics of meningococcal meningitis during the dry season (December to June), especially in the savannahs that stretch from Mali to Ethiopia. Vaccination is also indicated for those destinations where recent epidemics have occurred (as in the case of Chile and Mongolia).
Join our TRAVEL LETTER
Stay tuned
sconto del 10%
Error: No feed found.
Please go to the Instagram Feed settings page to create a feed.